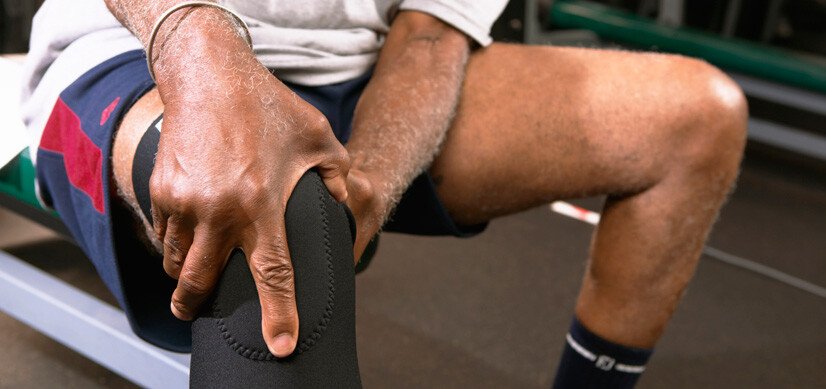
Leg heaviness at the end of a long day feels like an obvious consequence of being on your feet. Most people attribute it to tiredness, age, or standing too long — and most of the time they are right. But for a significant number of people, that familiar heaviness, aching, or swelling is not muscular fatigue at all. It is a vascular problem, specifically a problem with the veins. As a varicose vein specialist in Aurangabad, Dr. Amol Lahoti at dramollahoti.com sees patients every week who have been living with a treatable vein condition for years, assuming it was simply tiredness.
The challenge is that early varicose veins and chronic venous insufficiency do not always announce themselves with dramatic visible veins. For many patients, the first signs are subtle — a feeling of weight in the legs, mild swelling by evening, occasional cramping at night, or a persistent dull ache that improves when the legs are elevated. These symptoms overlap almost perfectly with general leg fatigue, which is why the vascular cause is consistently missed. Visit Dr. Amol Lahoti on Google to learn more and book a consultation.
Ready to consult? Book An Appointment with Dr. Amol Lahoti today.
Understanding the Venous System in the Legs
The legs have two sets of veins — superficial veins that lie just beneath the skin and deep veins that run through the muscle. Both systems are equipped with one-way valves that open to allow blood to flow upward toward the heart and close to prevent it from flowing back down. When these valves weaken or fail, blood pools in the vein rather than moving forward. The vein distends under the accumulated pressure, eventually becoming the twisted, rope-like structure visible through the skin that most people associate with varicose veins.
What is less understood is that valve failure can be present and causing symptoms long before visible varicosities appear on the surface. The underlying venous hypertension — raised pressure in the vein — produces the same symptoms of heaviness, aching, and swelling regardless of whether the veins are yet visible.
Varicose Veins vs Tired Legs — How to Tell the Difference
Symptoms That Point to a Vascular Cause
• Heaviness or aching that is consistently worse in the evening and significantly better after a night of sleep or after elevating the legs — this pattern of postural relief is a classic venous symptom
• Swelling of the ankles or lower legs that appears progressively through the day and resolves overnight
• Visible twisted or bulging veins on the thighs or calves, ranging from fine purple spider veins to large rope-like varicosities
• Itching or a crawling sensation over the affected vein
• Night cramps in the calves that disturb sleep
• Skin changes in the lower leg — darkening, thickening, or a brownish discolouration, particularly around the ankle
• A healed or active ulcer near the ankle in advanced cases
Symptoms That Are More Likely General Fatigue
• Leg aching that is diffuse, affects the muscles uniformly, and is directly proportional to physical activity
• Symptoms that are equal in both legs without any postural variation
• No visible vein changes and no ankle swelling
• Symptoms that resolve completely with rest regardless of leg position
• Pain that is sharp, localised, and worsens with specific movements — more consistent with a musculoskeletal cause
The most reliable distinguishing feature is postural relief. If your leg symptoms improve specifically when your legs are raised above heart level, that is a venous pattern. Muscular fatigue improves with rest regardless of position.
Ready to consult? Book An Appointment with Dr. Amol Lahoti today.
Risk Factors for Varicose Veins
Understanding whether you are at elevated risk helps contextualise your symptoms. The following factors increase the likelihood that your leg symptoms have a vascular cause:
• Family history — venous valve weakness has a strong genetic component. If one parent had varicose veins, your risk is approximately 40 to 45 percent. If both parents had them, the risk rises to around 90 percent
• Prolonged standing — occupations that require standing for most of the working day (teachers, healthcare workers, retail staff, factory workers) place sustained hydrostatic pressure on the leg veins
• Pregnancy — the growing uterus compresses pelvic veins, increasing venous pressure in the legs. Hormonal changes also relax vein walls. Varicose veins that develop during pregnancy may improve after delivery but often do not resolve completely
• Obesity — excess body weight increases abdominal pressure, which impairs venous return from the legs
• Previous DVT (Deep Vein Thrombosis) — damage to deep vein valves following a clot is a common cause of chronic venous insufficiency
• Age — valve function naturally declines with age, making varicose veins significantly more common after 50
Why Varicose Veins Are Not Just a Cosmetic Problem
The most common misconception about varicose veins is that they are primarily a cosmetic issue — unsightly but harmless. This is inaccurate, and it is one of the main reasons patients delay seeking treatment until their condition has progressed significantly.
Untreated varicose veins represent a progressive condition. The venous hypertension that causes the visible veins also causes ongoing damage to the skin and underlying tissue in the lower leg. Over time this produces:
• Lipodermatosclerosis: Hardening and thickening of the skin and fat tissue in the lower leg, making future treatment more complex
• Venous eczema: Inflamed, itchy, weeping skin over the varicose veins or around the ankle
• Pigmentation: Permanent brownish discolouration of the skin from haemosiderin deposits — iron released from red blood cells that leak through the distended vein wall
• Venous leg ulcers: Open wounds near the ankle that are notoriously slow to heal and frequently recur without addressing the underlying venous cause
• Superficial thrombophlebitis: Inflammation and clotting within a surface varicose vein, causing a painful, red, cord-like lump along the vein
• Bleeding: Varicose veins near the skin surface can rupture with minor trauma, causing significant bleeding that is alarming in proportion to its actual cause
When to See a Vascular Surgeon
Not every patient with mild spider veins requires immediate surgical intervention. But the following situations warrant a formal evaluation with a vascular surgeon rather than continued watchful waiting:
• Symptoms are affecting your quality of life — difficulty standing for normal periods, poor sleep due to night cramps, or significant daily discomfort
• Visible varicose veins that are enlarging or multiplying over months
• Skin changes appearing in the lower leg — discolouration, hardening, or eczema
• Any episode of superficial thrombophlebitis — a painful, inflamed segment of vein
• A history of venous ulceration or an active ulcer
• Significant ankle swelling that is new or worsening
At Dr. Amol Lahoti’s clinic, the evaluation begins with a detailed clinical examination and a venous duplex ultrasound — a non-invasive scan that maps the venous system in both legs, identifies which valves have failed, and determines the extent of reflux. This information is what drives the treatment plan. No two patients have identical venous anatomy, and treatment should reflect that.
Frequently Asked Questions
Q: Can varicose veins go away on their own?
No. Once venous valves fail, they do not recover function. Varicose veins do not resolve spontaneously. Compression stockings can manage symptoms and slow progression but do not treat the underlying valve failure. Only medical intervention addresses the cause.
Q: Are compression stockings enough treatment?
Compression stockings are an effective way to manage symptoms and are appropriate for patients who are not yet ready for intervention or who have contraindications to treatment. However, they do not eliminate the varicose veins, reverse the valve failure, or prevent progressive skin changes. They are a management tool, not a cure.
Q: I have had varicose veins for years with no ulcers or skin changes. Is it still worth treating?
Yes, for two reasons. First, the longer treatment is delayed, the more the skin and tissue in the lower leg are affected by chronic venous hypertension, making outcomes progressively less complete. Second, modern varicose vein treatments are minimally invasive, have very short recovery times, and produce excellent results. The risk-benefit calculation heavily favours early treatment.
Leg Heaviness, Swelling or Visible Veins? Get a Proper Answer.
Dr. Amol Lahoti, vascular surgeon, will assess your venous health with a clinical examination and duplex ultrasound and give you a clear treatment plan.
Visit dramollahoti.com or find Dr. Amol Lahoti on Google to book your consultation.
Ready to consult? Book An Appointment with Dr. Amol Lahoti today.
Google: Dr. Amol Lahoti on Google Maps | Treatment: Varicose Veins Treatment | About: About Dr. Amol Lahoti
